As a parent it can be difficult to identify even the most common baby rashes and spots on babies. So, let's look at the differences, how can you spot skin conditions and how to help soothes itchy skins and treat rashes on little ones.
Rashes are common in newborns and young babies as their skin comes into contact with new irritants and environments outside the womb. It's very normal to experience newborn skin peeling too, but knowing when this is eczema, baby hives, or another type of a rash can be tricky to work out. So we consulted an expert for advice.
If you are concerned about your baby, you should contact the NHS as soon as possible.
Baby rashes checklist
knowing when to worry about a baby rash is tricky, but important, which is why we've created this checklist to help you figure out when you need to call the GP to ensure your little one is safe.
Your baby has really delicate skin which can be easily irritated by products and ingredients. So, if you spot a rash emerging, then it could just be because something has aggravated them, but it’s still a good idea to run through this checklist to ease your mind that it’s nothing more serious.
We always advise that if you have any concern whatsoever, consult with your GP during the day, and call out of hours or emergency services if necessary.
Dr Tim Ubhi, a consultant paediatrician for the Royal College of Paediatrics and Child Health, has helped us out by providing some of the following information...
1. Does your baby have a temperature?
Take your baby's temperature and see what it reveals. According to the NHS a high temperature is 38°C and above. A high temperature and a rash combined could indicate your baby has measles and it’s advisable to see a GP.

2. Does your baby look unwell?
Trust your judgment and decide if you think your baby looks unwell (despite the rashes). If they look pale and sweaty, then try making sure they're not dehydrated by feeding them, or giving them water.
3. Have you tried the glass test?
Gently press the side of a glass to the patch of skin with the rash. If you can see the rash through the glass, then your baby may be showing signs of meningitis, which requires urgent medical attention.
4. Are they still feeding?
A good way to tell if a baby is unwell is by seeing if they'll still feed normally. If they don't want to feed, then give it a while and try again. If that doesn’t work, chances are they're not feeling right and it’s best to consult your GP.

5. Is their urine and poo output normal?
Check what’s in your baby’s nappy every so often. If they're feeding normally, your baby should have up to 10 wet nappies a day.
6. Are they too hot?
If your baby is sweating or their tummy feels hot, they may be overheating. Remove some layers and see if it makes a difference – the aim is to keep them from overheating.
7. Have you changed your baby’s nappy recently?
If the rash is surrounding your baby’s bottom, then chances are it is nappy rash, which can develop for a number of reasons. Try changing your baby's nappy and top and tailing your baby. Leave them to dry with no nappy on and apply some barrier cream.
8. Have you used a new skincare product or washing powder?
Lots of things can irritate your baby’s delicate skin – including your own perfume. Certain products or a change of products can lead to flare-ups of eczema and other skin conditions. Gently clean your baby and gently pat them dry, without applying any products. If the rash remains, baby eczema products may help.
Baby rashes to look out for
Chickenpox
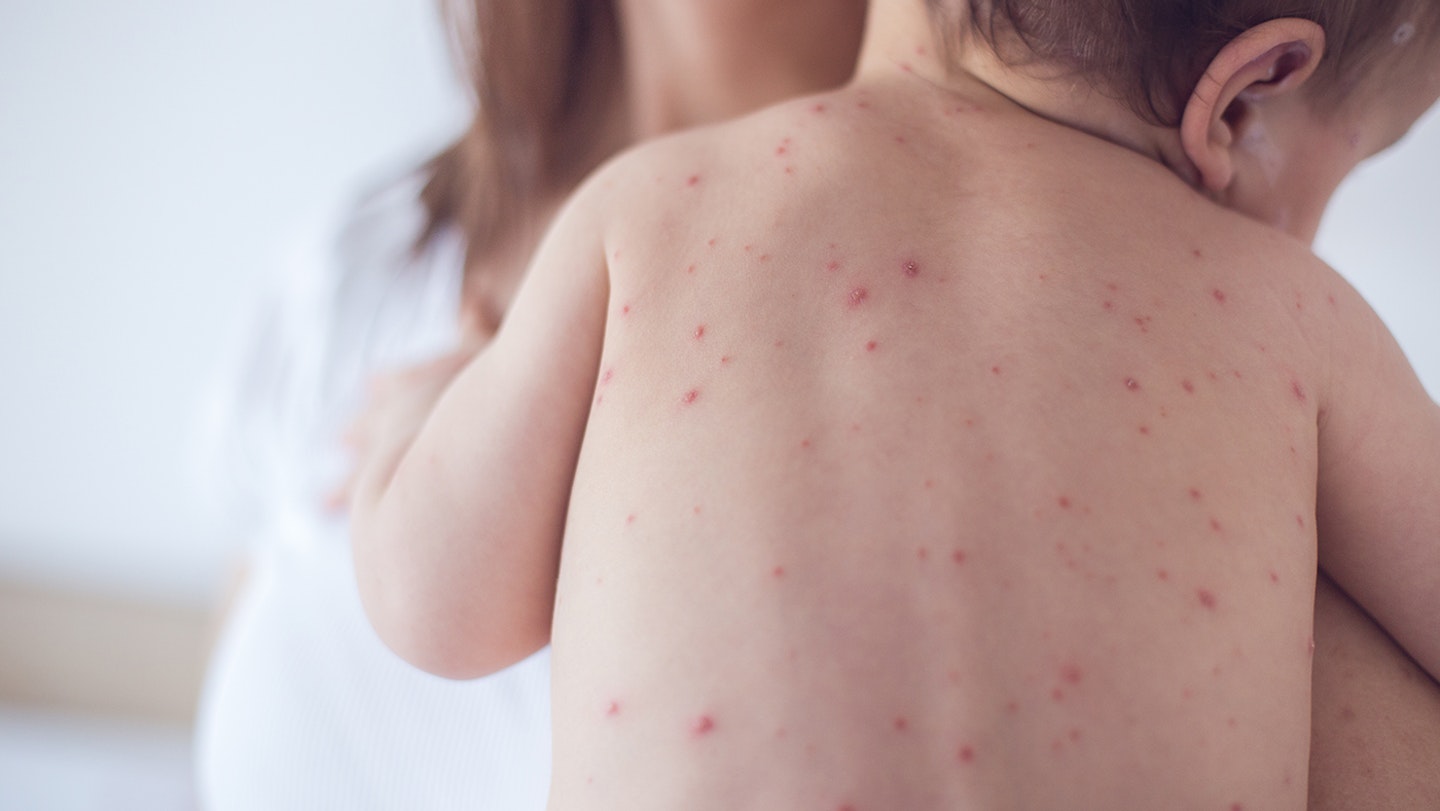
Chickenpox will affect 9/10 children in the UK, most of them before the age of four, according to research.
Chickenpox causes an itchy rash, spots and fluid-filled blisters, among other symptoms, and is particularly prevalent between March and May. Scratching can lead to further infections, sleepless nights and permanent scarring.
Before the rash appears, it’s common to experience mild flu-like symptoms, including feeling sick, a high temperature of 38°C or over, aching muscles and a headache.
“Chickenpox is a mild and common viral illness that seems to strike most children down at some point, particularly if they are in close proximity to other infants,” says Dr Sarah Jarvis, GP and clinical consultant.
“Look out for clusters of red spots, which turn into small, fluid-filled, itchy blisters that break and then scab over.”
This initial rash can be harder to see on black and brown skin, so Mini First Aid advise to look under the forearms and in the mouth and inside of eyes. Some children have only a few spots, but other children have spots that cover their entire body. Spots are most likely to appear on the face, ears and scalp, under and on the arms, chest, stomach and legs.
Key symptoms
-
Itchy rash
-
Spots
-
Fluid-filled blisters
-
High temperature
Cause: A virus called the varicella-zoster.
Heat rash (prickly heat)
“Heat rash, also known as miliaria or prickly heat, appears as tiny little red bumps or blisters on the skin and it happens when children get too hot. The rash often stings or feels prickly," explains Dr Sarah.
It can occur anywhere on the body, but often appears in places covered by clothing.
Heat rash presents as pink or red on white skin, but is difficult to identify on black and brown skin as the skin will not necessarily change colour, although it can look spotty. Instead, if your child is old enough, ask about symptoms: does your skin feel sore or itchy? Are you very thirsty? Watch out for signs of dehydration such as not producing wet nappies.
Key symptoms
-
Small, raised spots or bumps
-
An itchy, prickly feeling
-
Mild swelling
Cause: Excessive sweating.
Measles
"Measles is a type of virus called ‘paramyxovirus’ which can be contracted by an infected person’s saliva - so if they cough or sneeze near a child who is not vaccinated, they could breathe in tiny droplets and pick up the virus,” says Dr Sarah.
“Watch out for tiny white spots with a red outline inside the mouth, followed a few days later by a fine red rash that starts small and becomes blotchy.
“This rash appears after initial cold-like symptoms, such as red eyes, sensitivity to light, a fever and greyish white spots in the mouth or throat.”
The spots develop in the mouth and on the cheeks whilst the rash typically starts behind the ears and then spreads to the body. You should see your GP immediately if you suspect your child has measles.
Key symptoms
-
High temperature
-
Runny/blocked nose
-
Sneezing
-
Coughing
-
Red, sore, or watery eyes
Cause: A virus in the paramyxovirus family.
Eczema
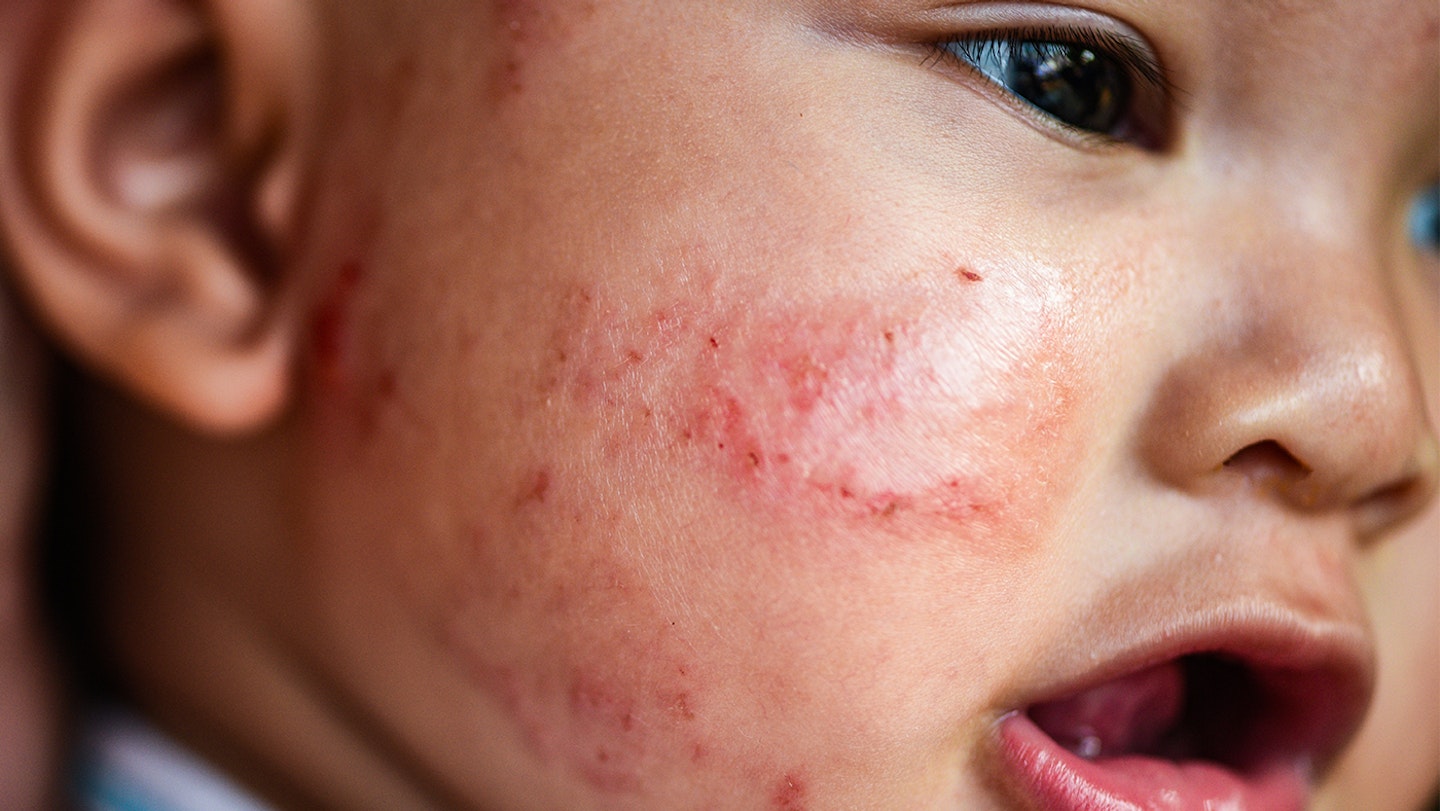
“Eczema can often be identified by a dry, red patch of skin that may be broken or cracked,” says Dr Sarah.
The most common form in children is atopic eczema, which presents as small areas of dry skin that are occasionally itchy. In some severe cases, atopic eczema can cause widespread dry skin, constant itching and oozing sores.
Eczema can occur anywhere on the body but in infants, you are most likely to see it on the face, arms and legs and in children on their hands, around their joints, such as the front of their elbows or the back of their knees.
Eczema can sometimes be confused with teething rash, so it's worth ruling that out too.
It can look less severe on black and brown skin, but this doesn’t mean it isn’t just as sore. Mini First Aid advise that eczema patches can look darker than skin colour, or even ashy grey in appearance. Where scratching has broken the surface of the skin, this will present as pink or red, and scabs may also be present.
Key symptoms
-
Itchy, dry, cracked and sore skin
Cause: Environmental factors such as weather, dust mites and pollen. Also, food allergies and certain fabrics.
Meningitis
Meningitis is an infection of the protective membranes that surround the brain and spinal cord.
The rash associated with meningitis is non-blanching (does not disappear under pressure) and presents as a “pinprick” rash or purple bruises anywhere on the body (not always present and can be difficult to spot on black and brown skin).
“The meningitis rash occurs when septicaemia (blood poisoning) has taken hold," says Dr Sarah. "It is a blotchy dark red rash that doesn’t disappear under a glass tumbler when pressed firmly."
However, according to Mini First Aid, DO NOT wait for the rash if you suspect meningitis. It is often one of the later symptoms to present and can indicate serious infection by the time it appears.
Also look out for blotchy skin, getting paler or turning blue on white skin, but with an ashy or grey appearance on black and brown skin. Also look for pale eyelids and blueness on the inside of the mouth.
“There will be other symptoms to look out for including high fever, cold hands and feet (even with a high fever) and a pale, dusky or blue colouring around the lips. Other symptoms include a tense or bulging soft spot on babies’ skulls, poor feeding, drowsiness or irritability, and a high-pitched cry.
“In older children, look out for neck stiffness, headache, fast breathing, leg pains and dislike of bright lights.”
If you suspect meningitis, you should ring 999 or take your child to the hospital immediately.
Key symptoms
-
Blotchy dark red rash, which doesn't disappear under a glass tumbler
-
High temperature
-
Cold hands and feet
-
Pale, dusky or blue colouring around the lips
-
Bulging soft spot on babies' skulls
-
High-pitched cry
Cause: A viral or bacterial infection.
Impetigo
There are two types of impetigo: bullous impetigo and non-bullous impetigo.
“Non-bullous impetigo is very common, particularly in children and especially in hot, humid weather," says Dr Sarah.
“It usually starts with small blisters that burst quickly to leave scabby patches on the skin. These can look like cornflakes stuck to the skin, but the skin underneath is red and inflamed. These crusty patches are small at first, around half a centimetre across, but slowly grow.”
It is usually found on the face and hands as it occurs most frequently on regularly exposed skin, but it can appear anywhere on the body. Impetigo can clear up without treatment within 2 to 3 weeks, but you should visit your GP to make sure your child doesn’t have another, more serious infection.
Key symptoms
-
Small blisters that leave scabby patches
-
Over time they may spread and be itchy
Cause: The skin becomes infected with bacteria.
Hand, foot and mouth
This disease causes a non-itchy red rash and sufferers often get mouth ulcers. Symptoms appear 3-5 days after being in contact with someone who’s affected.
“The rash on the hands and feet starts as small red spots but can sometimes then develop into uncomfortable blisters. It is very common in children under 10," says Dr Sarah.
“Hand, foot and mouth often starts with a fever of around 38-39°C, sore throat and sometimes loss of appetite, followed quickly by the appearance of mouth ulcers, then other spots.”
The spots and blisters on hands and feet develop soon after the blisters in the mouth. The raised spots can look pink, red or darker than surrounding skin, depending on your skin tone. The spots become blisters which appear grey or lighter in colour than the surrounding skin and can be painful and /or itchy.
As the name suggests, hand, foot and mouth appears on the hands, feet and in the mouth, but it’s not uncommon to get spots on the buttocks, legs and genital areas too.
Key symptoms
-
Sore throat
-
High temperature
-
Not wanting to eat
Cause: A virus spread in coughs, sneezes, poo and the fluid in the blisters.
Scarlet fever
"This is an extremely contagious bacterial illness that mainly affects children, although it’s less common than it was a few years ago," explains Dr Sarah.
“Scarlet fever is caused by a germ called streptococcus, it gives rise to a distinctive pink-red rash, which feels like sandpaper to touch and looks like sunburn.”
On white skin, the rash may present as pinky-red “pinpricks”, however, this can be difficult to spot on black and brown skin where the “pinprick” bumps may simply be skin-coloured. Mini First Aid advise that the key here is the texture of the rash – it will likely feel like sandpaper. “Strawberry tongue” can also be present with scarlet fever, so this is important to look out for as well – the tongue will look more red / purple than usual, and may have spots like strawberry seeds!
Scarlet fever usually starts with a sore throat and high temperature, followed within 12-48 hours by a rash. This usually starts on the chest and neck before spreading to other areas of the body, such as the ears and stomach, hands and feet.
See your GP as soon as possible if you suspect your child has scarlet fever.
Key symptoms
-
Flu-like symptoms
-
High temperature
-
Sore throat and swollen neck glands
-
12-48 hours later a rash will appear
Cause: A bacteria known as Group A Streptococcus.
About the experts
Dr Tim Ubhi is an NHS Consultant Paediatrician & Fellowfor the Royal College of Paediatrics and Child Health. He has over 29 years experience in Paediatrics & founded the Children's e-Hospital in 2015, this was the first online child health service of it's kind. The service has been rated "Outstanding" by The Care Quality Commission.
Dr Sarah Jarvis trained at Cambridge (1980-1983) and Oxford (1983-1986) universities and became a partner in an inner-city general practice in 1990. She is an active medical writer and broadcaster.
Maria Martin is the Online Editor for Mother&Baby and has won Bauer Media Awards for 2018 Digital Editor Of The Year and 2017 Digital Talent Of The Year. She is a biker, mama-of-one who enjoys baking and taking her little one to messy play. Maria's focus is around breastfeeding, post-partum depression and weaning. She aspires to help fellow mums through pregnancy, motherhood and beyond by discussing issues such as mental health and self-care.
