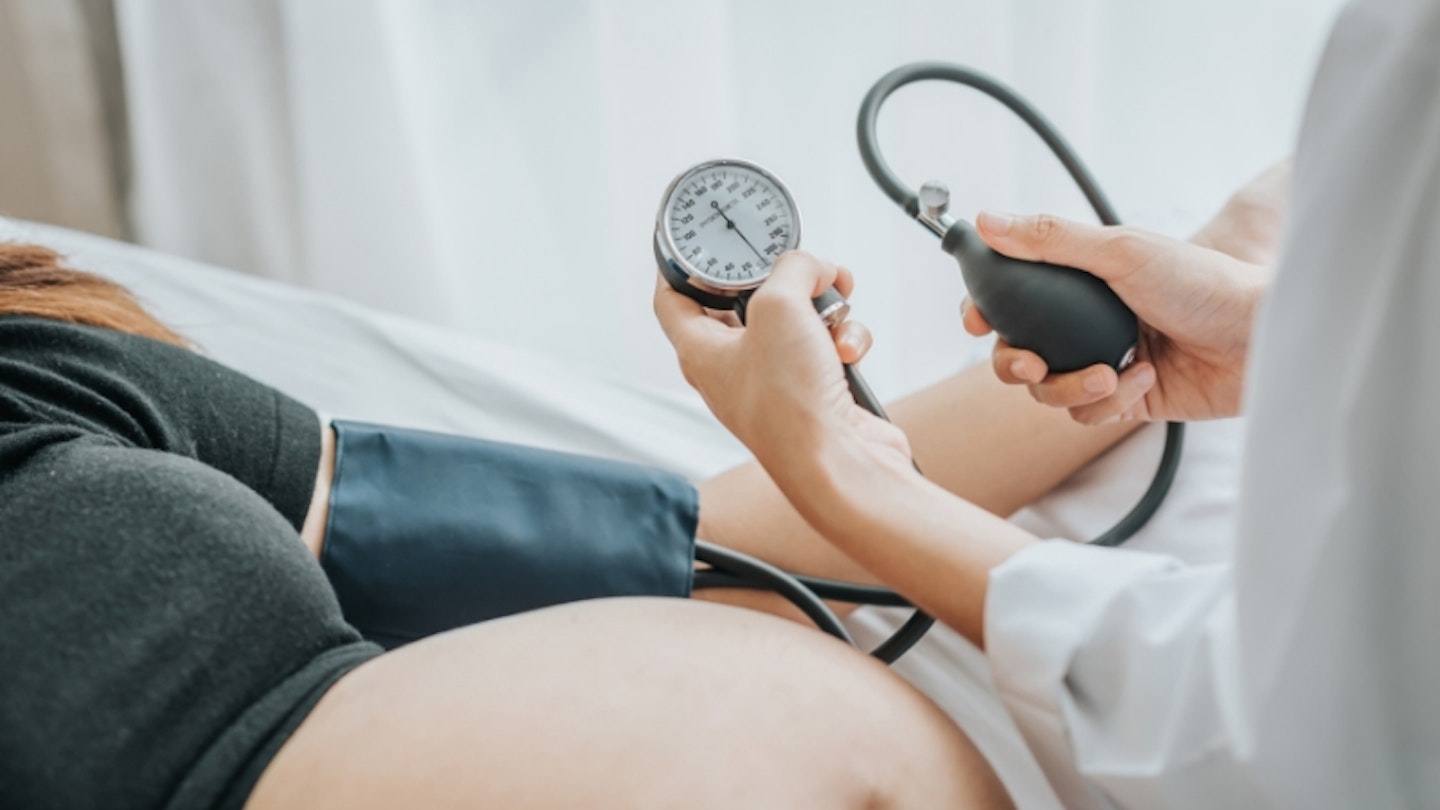
Along with a hefty list of side effects and symptoms like swelling, morning sickness and fatigue, pregnancy can also bring unwanted health conditions and complications. Symptoms that you try to shrug off could even be a tell-tale sign of something more serious. Pre-eclampsia is a condition that affects some people in pregnancy (usually after 20 weeks) or soon after their baby is delivered. It is a pregnancy and post-pregnancy health condition which sometimes appears without symptoms, but it can cause problems for you and your unborn baby.
Knowing what to look out for can help you get the treatment that you need so we explain what is pre-eclampsia, the causes, symptoms and treatments.
What is pre-eclampsia?
Pre-eclampsia is a condition that sometimes strikes during the second and third trimester of pregnancy (from around 20 weeks) or immediately after giving birth. According to the NHS "Mild pre-eclampsia affects up to 6% of pregnancies, and severe cases develop in about 1 to 2% of pregnancies."
It is thought to relate to a problem with the placenta. "Pre-eclampsia can cause a combination of high blood pressure (hypertension) and protein in your urine (proteinuria)" says Shreelata Datta, an obstetrician at St Helier Hospital in Surrey.
What are the causes of pre-eclampsia?
The exact causes are not fully understood, but the condition is thought to be caused by the placenta not developing properly due to a problem with the blood vessels supplying it.
There are certain things which can increase your chances of developing pre-eclampsia.
What tests and checks are there for pre-eclampsia during pregnancy?
You'll have appointments with your midwife throughout your pregnancy, and your urine should be tested at each routine check you have, as this is how pre-eclampsia can be diagnosed. At your antenatal appointments, a sample of your wee will be tested for protein; you may also be asked to take a wee sample with you, if you can. You may be asked for another sample for testing if the first test shows your wee has protein in it. Your blood pressure will also be taken at these appointments, and if it is too high, it may be taken again. If your midwife, doctor or consultant thinks you may have pre-eclampsia, you will be offered a blood test to check for a protein called placental growth factor (PIGF). If your PIGF levels are low, it could be a sign of pre-eclampsia.
Pre-eclampsia risk factors
Certain conditions/diseases
If you have diabetes, high blood pressure (known as hypertension in pregnancy) or kidney disease before starting pregnancy you are at a greater risk of pre-eclampsia.
Autoimmune diseases
If you suffer from an autoimmune disease such as lupus or antiphospholipid syndrome, it could increase the chances of developing pre-eclampsia.
Previously having pre-eclampsia
If you have developed the condition during a previous pregnancy then you are more likely to suffer from it again.
Family history
If you have a family history of pre-eclampsia such as your mother or grandmother suffering from the condition, this could make it more likely you will get the condition. Always inform your doctor of your family history and look out for symptoms.
Age
If you are over 40 years old it can increase the chances of pre-eclampsia. Anything over 35 is considered a geriatric pregnancy and can bring certain risks and complications.
Length of time between pregnancies
If it has been 10 years since your last pregnancy then you could be more at risk of pre-eclampsia.
Multiple babies
If you are expecting multiple babies (twins, triplets etc.) it can increase your risk of pre-eclampsia. A study in the Chinese Medical Journal found that the chance of pre-eclampsia in multiple pregnancies was 9.3% whereas for single pregnancies it is 1.8%.
Weight
Being overweight and having a body mass index (BMI) of 35 or over can increase the risk of pre-eclampsia.
What are the symptoms of pre-eclampsia?
There are often no symptoms with pre-eclampsia unless it’s severe, other than heightened blood pressure. Swelling is a common and typically harmless side effect of pregnancy but it can indicate also indicate complications like pre-eclampsia.
‘If your pre-eclampsia is severe, symptoms include bad headaches that aren’t eased with paracetamol, problems with your vision, such as blurring or flashing lights before your eyes, severe pain just below the ribs, heartburn that doesn’t go away with antacids, rapidly increasing swelling of the face, hands or feet or generally feeling very unwell,’ says Shreelata.
These are some known symptoms of pre-eclampsia:
High blood pressure (140/90 mmHg or higher)
Protein in the urine
Severe headaches
Changes in vision (including blurred vision, seeing spots or temporary loss of vision
Upper abdominal pain
Nausea or vomiting (especially if it occurs suddenly after mid-pregnancy)
Swelling (especially in the face and hands
Shortness of breath
How is pre-eclampsia diagnosed?
To find out whether have pre-eclampsia, your GP will take your blood pressure. If it is high, the next step would be looking for protein in your urine. You might then have further urine tests, or be referred to hospital for monitoring.
It is especially important to attend all antenatal appointments if you think you may be suffering from pre-eclampsia. ‘It may be picked up at your routine antenatal appointments when you have your blood pressure checked and urine tested,’ says Shreelata. ‘This is why it is always important to bring a urine sample to your midwife appointments.’
A new test known as the placental growth factor (PLGF) test, which checks the health of the placenta and can help spot preeclampsia in a day, will also now be offered to pregnant women on the NHS. The new guidelines will allow midwives to be able to use the test alongside other checks to quickly identify the condition.
Jeanette Kusel, from NICE told the BBC: "This is extremely valuable to doctors and expectant mothers as now they can have increased confidence in their treatment plans and preparing for a safe birth."
How is pre-eclampsia treated?
The only cure for pre-eclampsia is to give birth to your baby. Your GP might prescribe certain medication for high blood pressure. Women at risk of high blood pressure are often advised to attend the hospital two or three times per week to be monitored. There is a new app, The Hampton app, which has been recommended by the NHS. It allows women to check their blood pressure at home to prevent unnecessary hospital stays.
‘If you’re experiencing any of the symptoms associated with severe pre-eclampsia you should seek medical help immediately,’ says Shreelata. If in doubt, contact the maternity unit at your local hospital.
What is HELLP syndrome?
HELLP syndrome is sometimes thought to be a severe form of pre-eclampsia. This rare condition is a blood clotting disorder, meaning that the liver may be significantly injured.
The Pre-eclampsia Foundation explains: "HELLP syndrome was named by Dr. Louis Weinstein in 1982 after its characteristics:
-
H (hemolysis, which is the breaking down of red blood cells)
-
EL (elevated liver enzymes)
-
LP (low platelet count)
HELLP syndrome can be difficult to diagnose, especially when high blood pressure and protein in the urine aren't present. Its symptoms are sometimes mistaken for gastritis, flu, acute hepatitis, gall bladder disease, or other conditions."
How does preeclampsia affect the baby?
The consequences for your baby may vary widely from being just a day under close observation to having lifelong disabilities. However, complications can occur if your baby is delivered early to relieve your symptoms of pre-eclampsia. Most cases of pre-eclampsia pass with no effect on the baby.
Can pre-eclampsia occur after the baby is born?
If you have pre-eclampsia during pregnancy, after birth you are very likely to recover. You may need to rest in hospital for longer and you'll likely set up a plan with a midwife so your blood pressure can be monitored.
However, in rare cases, pre-eclampsia can occur after the baby is born. Symptoms are the same as pre-eclampsia, but it may be more intense. It usually occurs within the first 72 hours after giving birth, but in rare cases it can develop at any time during the first six weeks after birth. Seek medical help as soon as you notice any of the symptoms.
What is postpartum pre-eclampsia?
It is a rare but serious condition where high blood pressure and signs of organ damage (like protein in the urine) develop after childbirth, usually within the first 48 hours, but it can occur up to 6 weeks postpartum. The symptoms are similar to those of pre-eclampsia but can be more severe. Any of the symptoms mentions, especially severe headache, vision changes, chest pain, or difficulty breathing, after giving birth should be treated as an emergency. It's important to contact a healthcare provider or go to A&E immediately.
Pre-eclampsia FAQs
When do you go to hospital for pre-eclampsia?
You should seek immediate help if your blood pressure is reading very high, such as 160/110 or higher. If you are at home, you should call your hospital triage unit and will likely be asked to go in for monitoring. You should also seek help if you have these symptoms of preeclampsia: swelling of your face, hands, or feet and new vision problems (such as light sensitivity, blurring, or seeing spots).
Can stress cause pre-eclampsia?
High stress levels, depression and low mood can all have an effect on blood pressure. Stress isn't a direct cause of pre-eclampsia, but it can indirectly increase the risk of developing it by potentially leading to high blood pressure, which is a key symptom.
Can drinking lots of water prevent pre-eclampsia?
Pre-eclampsia is not fully preventable, but there are some life changes you can make to help lower your blood pressure. This could include drinking 6-8 cups of water per day and avoiding fried foods.
About the expert
Miss Shree Datta has over 17 years of experience in Obstetrics and Gynaecology, working in some of the top hospitals in London.
About the author
Hannah Mellin is Digital Writer at Mother & Baby. Her career at Bauer Media began ten years ago when she started as a freelancer and she has been writing for loads of our brands, interviewed celebrities, influencers, medical experts and more over the years. Hannah is a mama to a one year old little boy and is up for trying anything and everything to make mums feel less anxious and overwhelmed.