Welcome to my blog on the rollercoaster that is new fatherhood.
I’m Jim, my wife’s name is Daisy, I turned 51 last September and Daisy is a spritely 38. We had our first child in October 2022 – hence this, The Geriatric Dad Blog!
This is a proper, ‘in real life’ read from a man's perspective, so I hope you enjoy it and follow the series as we go – part 1 birth experience and part 2 birth experience.
This time: our son is born via an unplanned c-section...
"We advise a c-section as soon as possible"
It was the early hours of Monday morning on October 17th, 2022.
Daisy had been in labour since Friday morning and, finally, everything was coming to a conclusion, though not in the way we'd wanted. It had become clear our son could not be born vaginally. Daisy had started to bleed heavily into her catheter, while a sensor clamped to Mr Sprout's (our son's nickname) scalp fed data to monitors that indicated he was going downhill fast.
His pulse was slowing and he was becoming less active. The periods when he was 'awake' were becoming shorter and shorter. All this prompted the midwife to call the registrar, who appeared promptly.
They calmly analysed the data in hushed whispers before the registrar disappeared to call the obstetrics consultant, saying she'd be back soon. No doubt she wanted a second opinion, and quickly.
Once the second opinion was sought out and less than five minutes later, she came back into the birthing room to talk to us and advise us on what should happen next.
"The blood in the urine tells us there's likely a blockage, probably caused by baby's head pressing increasingly firmly against the bladder.
"While there isn't an immediate threat [to life] we feel the time has come to intervene as soon as possible.
"I've spoken to the consultant and we agree that baby's condition is deteriorating," she said calmly.
"So we'd advise an immediate C-section."
C-section risks
For someone who has a high degree of anxiety, I didn't actually feel that worried.
The medical team at Hinchingbrooke Hospital (in Huntingdon) were superb. They communicated clearly and calmly and made us both feel well looked-after and reassured.
We'd heard stories from other hospitals where birthing mothers had to share a single midwife, but not here.
I was calm and collected, for the time being at least. Of course, every decision was ultimately made by us, based on medical advice given.
"A C-section is major surgery that carries risks in its own right, to both mother and baby," continued the registrar.
She quickly ran through some of those risks, which included increased chances (for Daisy) of:
-
Severe haemorrhage (bleeding) that could be life-threatening
-
Pulmonary embolism
-
Sepsis (infection)
Daisy, who remained pain-free following an epidural the previous day, and I talked about what to do. We did our final assessment on the options presented to us, using the BRAIN acronym for the last time:
-
Benefits (of c-section now): best chance of getting baby out safely, best chance of Daisy surviving birth
-
Risks: it's major surgery. Daisy could bleed out, or get an infection (both small risks, but risks all the same)
-
Alternatives: hope the medics were incorrect with their assessment and wait to see if we could still achieve a natural birth
-
Instinct: our instincts told us strongly to give approval to proceed with the c-section
-
Nothing: doing nothing would likely result in Daisy and Mr Sprout dying...
So we agreed to the C-section and gave the necessary approvals. While it was the last option on the birth-plans we'd written, after a) normal birth into a pool, b) vaginal birth with gas and air, and c) vaginal birth with epidural, we felt we had no choice.
It was a no-brainer. What we were facing wasn't quite an immediate threat to either baby's life, mother's, or both - but it was urgent, and time to act to prevent escalation.
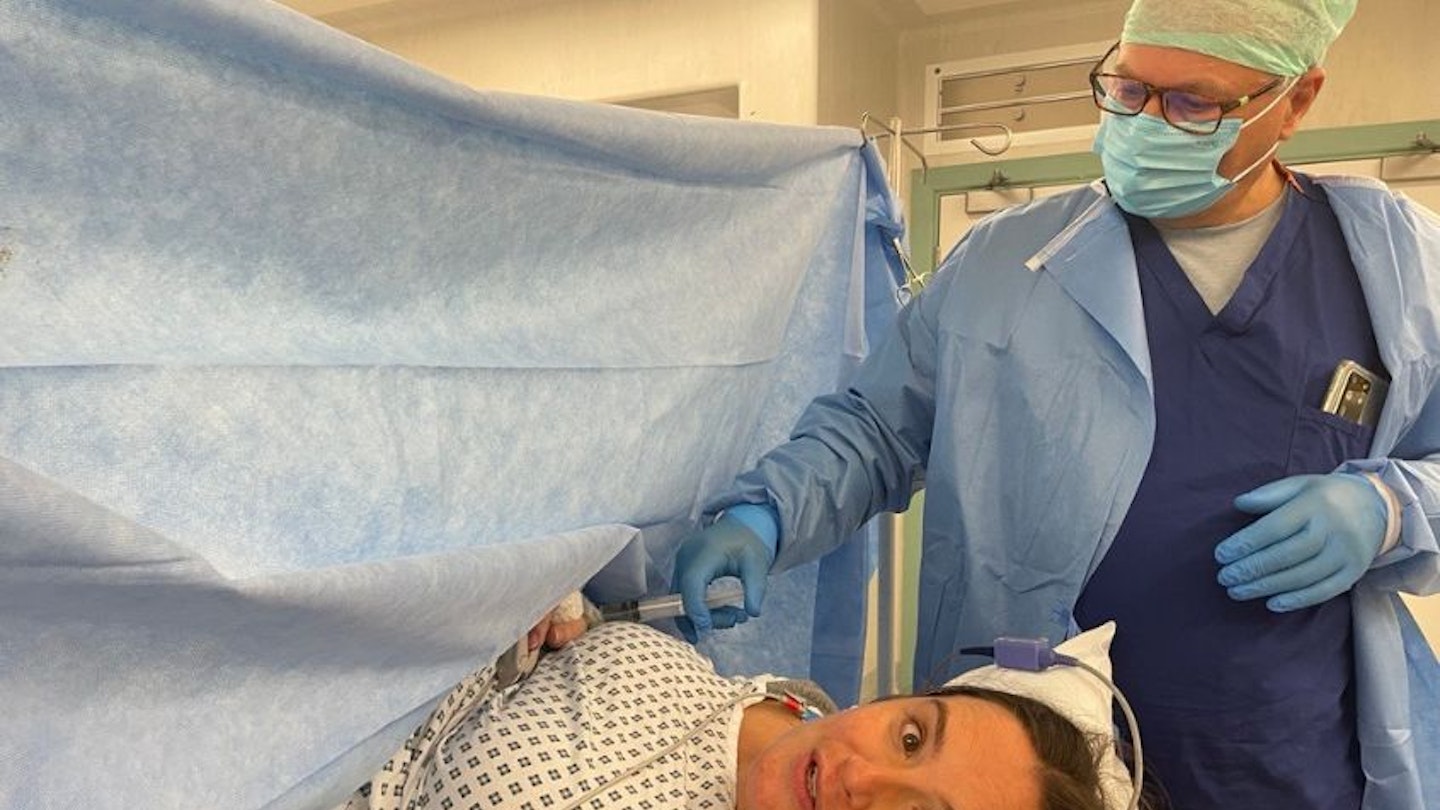
Daisy is wheeled into theatre
As soon as we'd given our OK, the birth room became a hub of activity. Medical staff were buzzing about calmly, each knowing their role, communicating in hushed tones with plentiful smiles. Friendly faces abounded as they got Daisy ready.
Some 20 minutes later, she was wheeled down the corridor and into the operating theatre, me walking by her side now in scrubs ready for the surgery.
I held her hand tightly and did my best to reassure her. She was excited, like me, at the prospect of meeting our son. A lady greeted us as Daisy and her trolley were positioned under those big lights you get in operating theatres.
I remember her big, friendly smile as she introduced herself as the theatre manager (or something similar, I can't quite remember). She was responsible for the smooth running of the theatre and the administration of the c-section ops that might come her way during her shift.
She ran through what was happening and introduced us to the team. There were loads of people in the room, far more than I was expecting. As they finished their preparations, we said hello to each and every one of them and, in the process, were told what their role was.
I believe we had with us...
-
Theatre manager
-
Two midwives
-
An obstetrician registrar
-
Obstetrician's assistant (junior doctor)
-
An anaesthetist
-
A resuscitation team
-
An anaesthetic nurse / operating department assistant
-
A scrub nurse
-
Two or three further theatre nurses
...though I could be wrong (apologies to Hinch if so!)
"Would you like us to film the birth?"
A screen was put up so Daisy couldn't see what was happening and I was given the option: would I like to sit behind the screen with Daisy, or watch the birth from the other side?
I wasn't expecting to have the latter option, so was a tad surprised it was offered!
While I was seriously interested to observe the operation, I thought it would be better to hold Daisy's hand and reassure her as events unfolded.
With that, the head midwife offered to film the whole thing for us on my phone, so I handed it over and let her get on with it, reminding her that we wanted a delayed cord clamping and cutting. Daisy also wanted to have as much skin-on-skin time with baby immediately after the birth as was possible.
Delayed cord clamping
There's a lot of thinking and scientific evidence as to why delayed cord clamping (DCC) is good for baby.
Some of the reasons include:
-
It allows extra blood to flow from the placenta into the baby
-
Increases the amount of iron passed to the baby
-
Helps keep baby's blood pressure stable
The head midwife agreed to do what she could, though I wasn't allowed to cut the cord (for unknown reasons I didn't want to argue with). The registrar then applied iodine to Daisy's belly and, when ready, made a horizontal incision along her bikini line.
The C-section
We were treated to a commentary as to what was happening from various team members on the other side of the 'curtain'. There was rather a lot of pushing and pulling on Daisy's belly from (I assume) a midwife.
I was surprised at the force used to push baby downward, from the top of Daisy's abdomen just below the rib cage. When I watch the video back, it amazes me every time.
"The baby's head is out!" someone cried.
The pushing and pulling continued, and when he was in a position where he could be grabbed, the registrar did indeed grab Mr Sprout and start to pull him out. Before his legs were even out of the womb, he embarked on his first-ever meltdown (there have been many since) screaming the theatre down.
But we didn't care. It showed he was healthy and his lungs were good, being filled with oxygen-rich air.
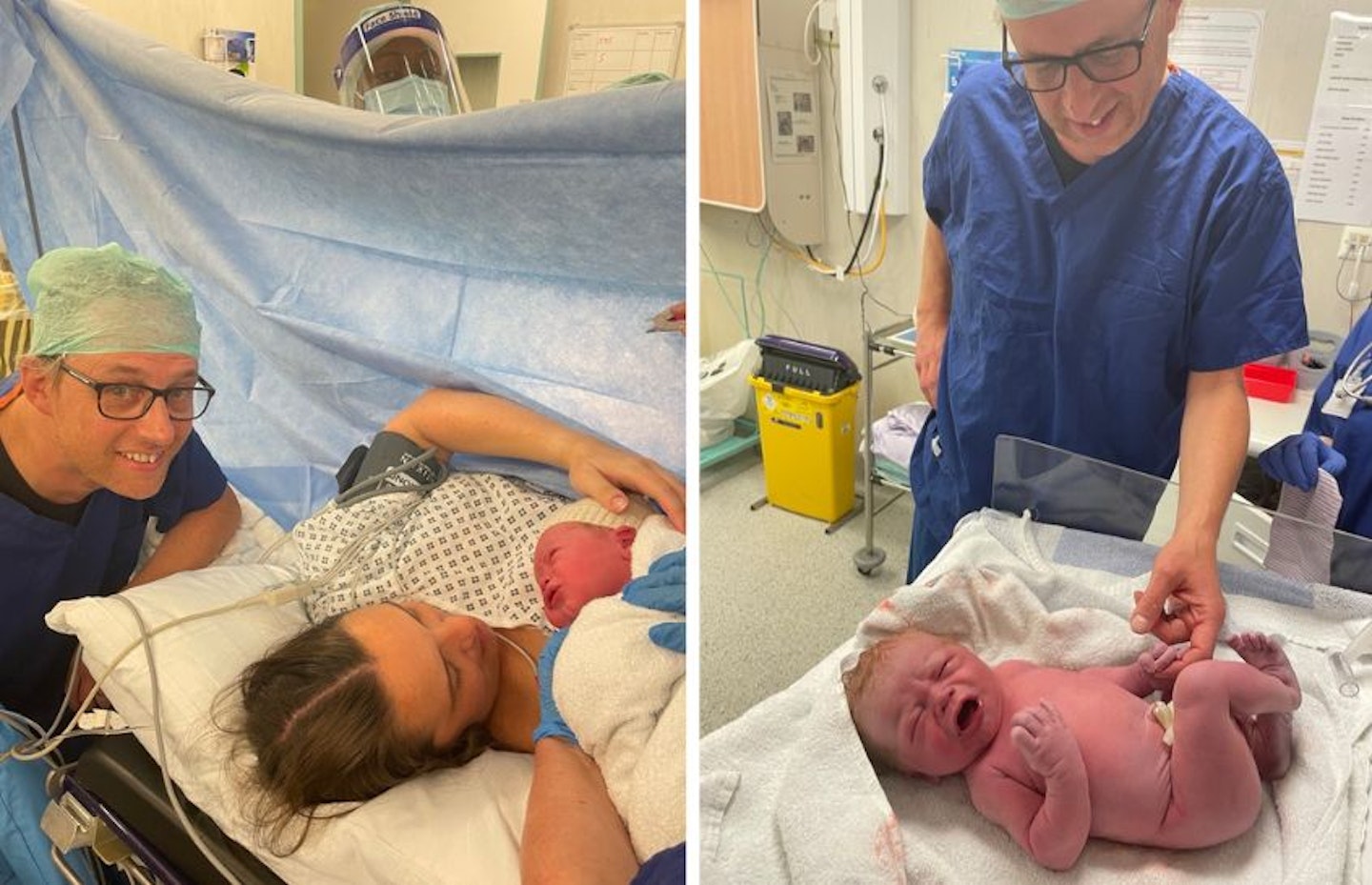
"He's blond!" exclaimed one of the midwives excitedly as he was finally and fully lifted from Daisy's stomach, umbilical cord trailing behind. Neither of us were expecting a blond baby! Daisy has Mediterranean genes and is fairly dark skinned with dark eyes, so it was not what we were expecting.
The registrar lifted Mr Sprout up above and then to the side of the screen, so we could see and meet him for the first time. Very briefly, Daisy and I both had some skin-on-skin with him before he was taken away to be weighed, have various medical checks, be swaddled and have a woollen hat put on his tiny head.
The cord-clamping was delayed as requested, but not for as long as we wanted, as I think (in retrospect) because Daisy was starting to haemorrhage.
While the registrar and her team began the process of stitching all the internal bits up, I was ushered over to the scales to see him weigh in at 8lb 14oz. He was a big baby, but not as big as we'd thought he might have been (at one stage it was estimated he'd be between 10 and 11lb, which shows how inaccurate estimations of baby-size can be from scans!)
My wife starts to haemorrhage
I went back to sit with Daisy as the medical team continued stitching her up internally, holding her hand as they did so. Mr Sprout was in good hands elsewhere in the room.
What happened next was frightening for me as a helpless dad and husband, looking on.
A minute slowly turned into five minutes, then 10. The operating theatre quickly went very quiet, the team communicating with each other in tones so hushed I could barely understand what they were saying.
The atmosphere became noticeably tense.
Daisy started to feel unwell. "I think I'm going to pass out," she told me on two occasions. Her face had gone very pale, a pallid grey hue coming over it. This was not the colour of a healthy person in the prime of life.
"Don't do that," I told her. "Stay with us." The hurried click of surgical tools, the whispered instructions, the ticking of a clock. Time. Moved. So. Slowly.
A request was made for Daisy to receive fluids, possibly saline or plasma, I can't remember (I guess to bump up her blood pressure). Repeated requests, one after the other, came in for gauze sponges to help control the bleeding.
Someone suggested they may need some O-negative blood, in case Daisy needed a transfusion. While I'm not a medical person, I knew enough to realise that my wife was haemorrhaging, maybe quite badly, and that the team were doing their best to control the bleeding.
Blood-soaked gauze sponges
Just 20 minutes previously I'd met my son for the first time and was euphoric. Now it felt like there was a real chance I might lose my wife. The euphoria was long gone, replaced by emotions that were the polar-opposite - fear, anxiety, a welling panic, and helplessness.
I took a glance around the side of the curtain to see what I could see. Several crimson-red gauze sponges met my eyes, each one completely soaked with Daisy's blood, in a pile.
I quickly poked my head back inside the protection of the curtain and tried to quell my burgeoning fear.
"Is everything ok?" Daisy asked slowly and quietly, as if it had been an effort to process and mutter just three words. Her head lolled slightly to one side, eyes vacant and to the back of their sockets, more white visible than coloured iris.
"Yes," I replied. "Everything is good, they're stitching you back up and Mr Sprout is asleep with one of the midwives."
It was a slight lie. I didn't feel everything was good, and I didn't know who had our son. I was scared, but throughout it all, the theatre team were arch professionals. Simply superb, each and every one of them.
We were reassured, while the anaesthetist watched Daisy's vital signs (blood pressure, heart trace) and topped up her drip from time to time. The surgical team just got on with what they had to do.
After what seemed an age, I started to hear counting. This was a good sign, as it meant the bleeding was likely under control and had been stopped. The surgical team were counting the number of used, blood-soaked gauze sponges they had piled up against the number logged that had been taken and used.
This simple procedure guards against materials being left inside Daisy – it's imperative all the gauze sponges, all the surgical tools used etc., are accounted for outside her body before the final stitches go in and she's closed up.
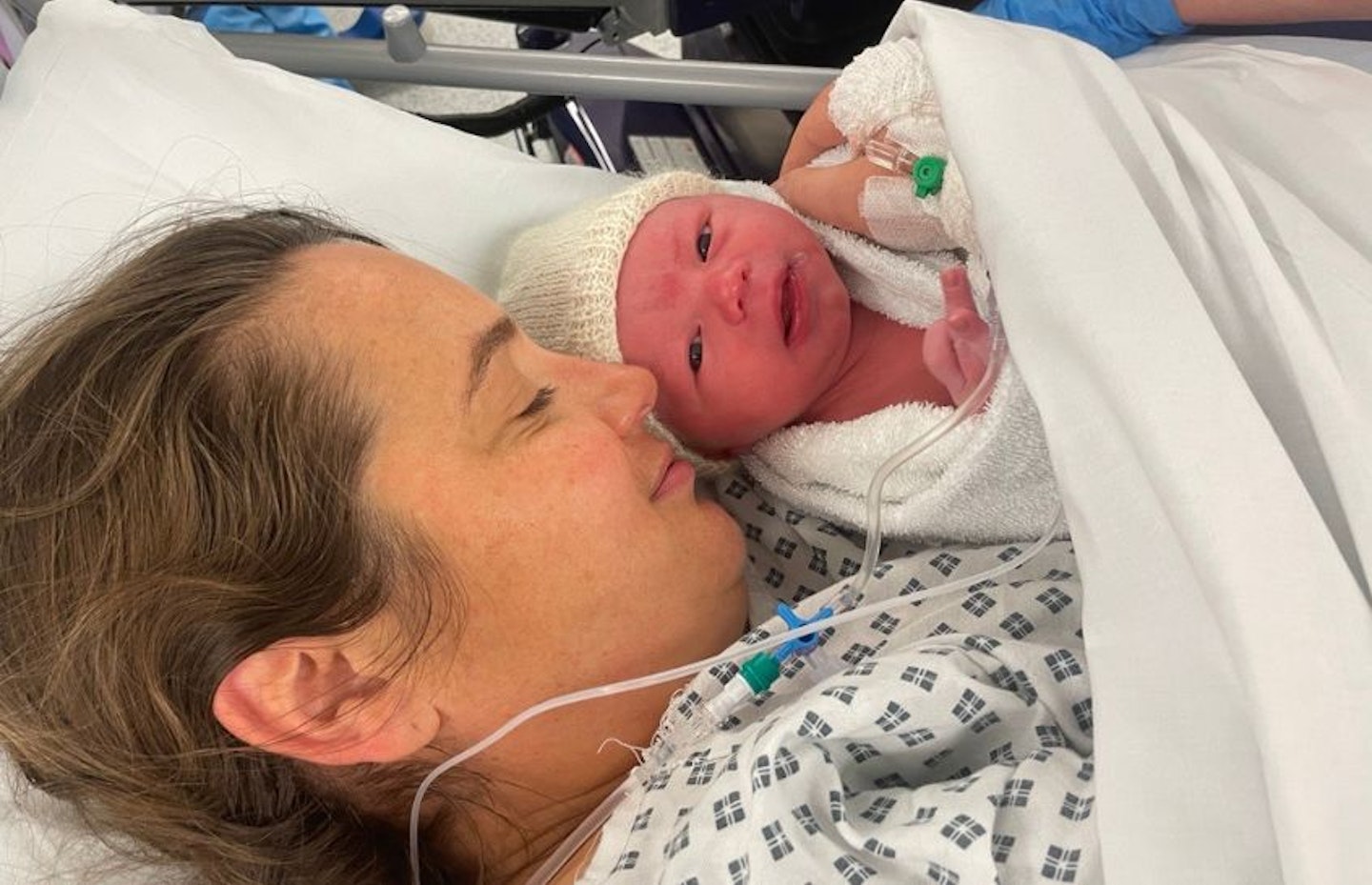
Then, it was all over and the wound had been closed. Everybody started to talk normally again, everybody visibly relaxed. We were reintroduced to our son, who as yet didn't have a name. Just Mr Sprout, for the moment. He was a picture of serenity, snuggled in a warm woollen cardigan and hat.
We were parents and our lives had just changed... forever.
NOTE: I'm not a medical expert! So if I have any of the above wrong technically, then apologies to the staff at Hinchingbrooke Hospital. You were fab and we owe you so much. Thank you!
Next time...
First nappies. First breast feed. Getting Mr Sprout to latch, and how to cope with your first night at home with a newborn following a c-section.